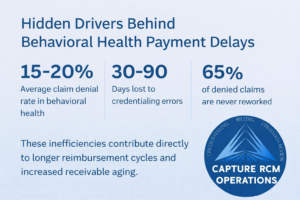
Payment delays are one of the most persistent financial pressures in behavioral health organizations. While claims may eventually be reimbursed, extended turnaround times compress working capital, disrupt forecasting, and limit growth.
Unlike simple billing errors, delayed payments in behavioral health often stem from structural breakdowns — authorization gaps, documentation inconsistencies, denial follow-up delays, or payer-specific nuances that slow reimbursement cycles.
For billing directors and operational leaders, reducing payment lag is less about overhauling the entire revenue cycle and more about tightening specific workflows that directly impact turnaround time.
Why Payment Delays Are More Common in Behavioral Health
Behavioral health billing operates under a different set of pressures compared to many other specialties.
Organizations frequently navigate:
- Prior authorization requirements tied to level of care
- Medical necessity documentation reviews
- Frequent plan reauthorizations
- Managed Medicaid complexity
- Variable payer turnaround timelines
- High denial scrutiny
These factors increase the number of checkpoints between service delivery and reimbursement. Each checkpoint adds potential friction — and friction creates delay.
The Most Common Drivers of Delayed Reimbursement
When payments extend beyond 30–45 days, the issue typically traces back to one of several operational gaps.
1. Authorization Breakdowns
Missed or incomplete authorizations often push claims into pending status. Even small documentation inconsistencies can stall processing.
2. Documentation Lag
Delayed clinical note completion slows claim submission and increases the likelihood of medical necessity denials.
3. Denial Follow-Up Gaps
Without structured follow-up protocols, denied claims drift into older receivable buckets, compounding recovery time.
4. Payer-Specific Submission Errors
Behavioral health billing rules vary widely across commercial and Medicaid plans. Small coding or modifier inconsistencies can trigger reprocessing cycles.
5. Credentialing Misalignment
Claims submitted before provider enrollment completion can remain unpaid for extended periods.
These issues rarely exist in isolation. Most organizations experiencing payment delays are managing overlapping inefficiencies.
Early Indicators That Payment Delays Are Becoming Systemic
Payment lag often worsens gradually. Billing leaders should watch for:
- Days in A/R steadily increasing quarter over quarter
- Rising 60- and 90-day receivable percentages
- Growing volume of pending or pended claims
- Increasing denial resubmission timelines
- Cash collections that fluctuate unpredictably
When these patterns emerge, delay is no longer incidental — it’s structural.
Practical Steps to Shorten Payment Turnaround
Reducing payment delay does not always require sweeping operational change. Often, targeted improvements produce measurable results.
Standardize Authorization Tracking
Create real-time dashboards that monitor upcoming expirations and pending approvals.
Accelerate Documentation Feedback Loops
Align clinical and billing teams with clear submission deadlines.
Implement Structured Denial Follow-Up Cadence
Daily payer follow-up rhythms prevent denials from aging unnecessarily.
Establish Payer-Specific Protocols
Maintain payer rule libraries to reduce rework cycles.
Assign KPI Ownership
Track metrics such as clean claim rate, denial rate, and average reimbursement timeline with defined accountability.
When oversight becomes consistent and data-driven, turnaround times begin to stabilize.
For organizations experiencing sustained delay across multiple areas, a more coordinated billing infrastructure — supported by structured behavioral health revenue cycle management oversight — may be necessary to restore predictable cash flow.
Why Addressing Payment Delays Early Matters
Extended reimbursement cycles don’t just affect accounting. They influence:
- Staffing decisions
- Hiring timelines
- Marketing investment
- Vendor relationships
- Expansion strategy
In multi-location behavioral health organizations, even modest increases in delay can compound across facilities and programs.
Proactive workflow adjustments prevent delay from escalating into financial instability.
The Bigger Picture
Payment delays in behavioral health are rarely about one isolated claim. They reflect how well front-end verification, clinical documentation, claim submission, denial management, and follow-up workflows operate together.
Organizations that treat payment lag as a solvable operational variable — rather than an unavoidable industry reality — often regain control over cash flow faster than expected.
For billing directors and operational leaders, the goal isn’t perfection. It’s consistency.
And consistency shortens the gap between service delivery and reimbursement.
Ready to Improve Your Cash Flow?
Don’t let payment delays control your practice. With Capture RCM, you get expert support, faster reimbursement, and peace of mind.
Call (380) 383-6822 or visit to see how our Behavioral Health Revenue Cycle Management services can transform your revenue strategy.